Retinal Exam and Consultation
A healthy retina is essential to maintaining clear vision and overall eye functioning. A retinal exam may be recommended by your doctor if any potential retinal abnormalities were detected during a general eye exam, or for patients at a higher risk of developing retinal conditions such as macular degeneration, diabetic retinopathy, retinal detachments and more.
During a retinal exam and consultation, one of our doctors will perform a series of diagnostic procedures in order to evaluate the retina for any sign of disease or abnormality. These tests may include Fundus Photography, Fluorescein Angiography, OCT, Visual Field and more.
Our doctors will take the time to discuss the results of your exam, as well as any potential risks of retinal disease with you. Patient education and understanding is a top priority of our practice, as it often helps patients achieve the most successful outcome.
Retinal Photography
Retinal photography is an advanced diagnostic tool that can be used to effectively detect and diagnose a wide range of abnormalities within the retina, the light-sensitive tissue that lines the back of the eye. These photographs can be used to evaluate the health of the optic nerve, vitreous, macula, retina and surrounding blood vessels, to diagnose conditions such as:
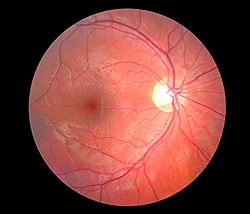
- Macular degeneration
- Diabetic eye disease
- Hypertensive retinopathy
Retinal photographs are taken during a simple, painless procedure using a high resolution camera and a specialized optical system.
Retinal photographs can help track any changes within the retinal tissue that may indicate early signs of a disease. They can also be used to track the progression of certain diseases. It is important for patients to have routine photographs taken so that any abnormalities can be detected as soon as possible.
Fluorescein Angiography
Fluorescein Angiography is a technique for examining the circulation of blood vessels inside the retina (an angiogram) with the help of a contrast dye (fluorescein dye). These pictures help doctors evaluate the retina and diagnose and track problems such as diabetic retinopathy, macular degeneration, abnormal vessel growth, swelling, leaking, retinal detachment, cancer or tumors.
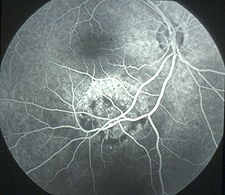
First, the patient's pupils are dilated with eye drops. Then a few photographs are taken with a special ophthalmic camera. Next, the contrast dye is injected, usually in the patient's arm. The dye travels up to the eye within a few seconds and "lights up" the blood vessels for the camera. Once the dye is in place, the doctor will take more photographs. Then the needle is removed. After about 20 minutes, a final set of photographs is taken for comparison.
Optical Coherence Tomography
Optical Coherence Tomography (OCT) is a non-invasive diagnostic test that obtains an extremely high resolution, cross sectional image of the retinal tissues. OCT is used to measure retinal and macula thickness and is very useful in detecting retinal swelling or fluid accumulation secondary to a variety of retinal conditions.

It provides very valuable information and is also useful for following the response to a treatment. OCT testing has become a standard of care for the assessment and treatment of most retinal conditions. OCT uses rays of light to measure retinal thickness and can be performed in a few minutes. No radiation or x-rays are used in this test.
Laser Retinal Surgery
Laser retinal surgery can be used to treat a wide range of retina conditions through minimally invasive techniques that produce precise, long-lasting results. Although your eyes may look and feel normal with these diseases, they can often lead to serious complications such as hemorrhaging and blindness.
Lasers have been used to treat eye diseases for over 30 years and produce effective results with no damage to surrounding tissue and no need for needles. It has quickly become the standard for eye disease treatment.
Laser surgery can be used to treat diabetic retinopathy, retinal vein occlusions, age-related macular degeneration, retinal detachments and more. Depending on the patient's condition, the laser may be used to seal leaking blood vessels, repair tears, remove newly formed blood vessels or destroy tumors. These procedures are performed in the doctor's office and require only anesthetic eye drops to numb the area prior to treatment. Laser treatment usually takes less than 30 minutes to perform, and patients can go home immediately following surgery. Most patients return to work and other normal activities the next day.
Several laser treatments may be needed in order to achieve optimal results and to help manage chronic retinal conditions. Results may take a few weeks or months to become noticeable, so it is important to see your doctor for follow-up appointments in order to ensure that you receive the best possible results.
Photodynamic Therapy
Photodynamic therapy is used to treat a complication of "wet" macular degeneration in which leaks form beneath the retina. These leaks occur in a structure in the eye called the choroidal neovascular membrane, or CNVM. During photodynamic therapy, Visudyne (verteporfin) dye is injected into the CNVM and a narrow-wavelength laser beam is focused on it for about 90 seconds. The dye absorbs the energy and slows or stops leakage by creating blood clots and stopping abnormal blood vessels from growing. Following treatment, patients should avoid direct exposure to sunlight for several days. Patients most likely to benefit from treatment will have newly onset macular degeneration and no scarring. Vision stabilization is maximized with a series of treatments over one to two years.
Intravitreal Injections
Intravitreal injections are commonly used to treat retinal diseases such as diabetic retinopathy, macular degeneration, macular edema, macular hole, and retinal vein occlusion. These diseases may cause loss of vision and should be treated as early as possible. Medications such as Lucentis, Avastin, Eylea, Ozurdex, and Jetrea can be injected directly into the eye to help patients maintain their vision and keep vision loss at a minimum. Some patients may see an improvement in their vision from these injections as well, depending on the condition being treated.
Intravitreal injections are especially effective in treating wet age-related macular degeneration, which, although less common than the dry form, accounts for more than 90% of blindness caused by the disease.
This procedure is performed in our office and requires only a local anesthetic. Before the medication is injected, the eye is numbed with anesthetic eye drops to help minimize discomfort. The eye is then cleaned with an antiseptic solution. The medication is then injected directly into the eye. Intravitreal injections may be administered as frequently as once a month, depending on the condition being treated, in order to maintain eye health and optimize the vision.
If you are interested in learning more about any of these conditions or our services and procedures, call 718-575-8434 today to schedule an appointment.